Northern Idaho hospitals permitted to save beds and ventilators for those 'most likely to survive'
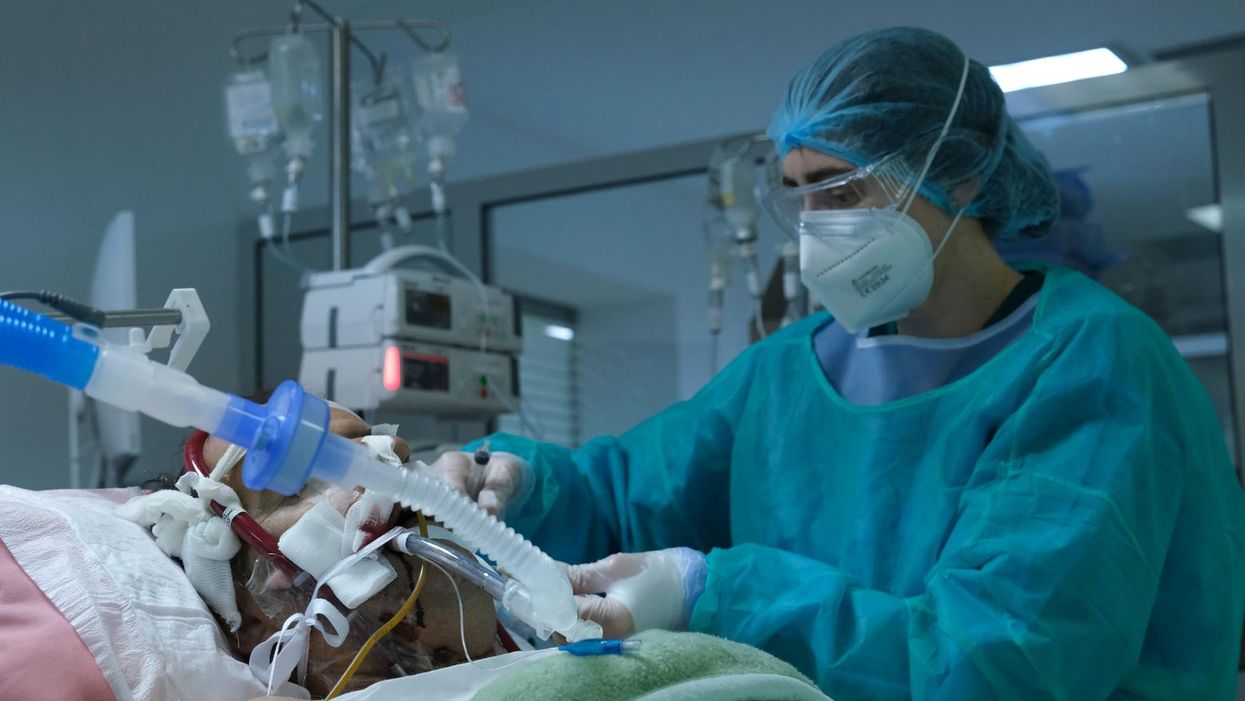

As hospital workers desperately try to save lives with limited resources and dwindling available beds during the COVID-19 pandemic, public health officials Idaho activated a "crisis standards of care" for northern hospitals last week that would in rare cases allow hospitals to save beds and ventilators "for those who are most likely to survive," The Associated Press reported of the guidelines dated last year.
"Crisis standard of care is a last resort," Idaho Department of Health and Welfare Director Dave Jeppesen said in a statement the AP obtained. "It means we have exhausted our resources to the point that our health care systems are unable to provide the treatment and care we expect."
Jeppesen added: "This is a decision I was fervently hoping to avoid. The best tools we have to turn this around is for more people to get vaccinated and to wear masks indoors and in outdoor crowded public places. Please choose to get vaccinated as soon as possible—it is your very best protection against being hospitalized from COVID-19."
Coronavirus cases in Idaho, a state with one of the country's lowest vaccination rates, have spiked in recent weeks. The state health department detailed "a severe shortage of staffing and available beds in the northern area of the state caused by a massive increase in patients with COVID-19 who require hospitalization."
Republican Gov. Brad Little said the state had reached an "unprecedented and unwanted point" in its history. "We have taken so many steps to avoid getting here, but yet again, we need to ask more Idahoans to choose to receive the COVID-19 vaccine," Little said in a statement. He didn't specify those steps, and many wonder what the governor is doing to protect his constituents.
Idaho had more than 600 patients hospitalized with COVID-19, and only 40% of residents vaccinated as of a New York Times report on Monday. "Washington State is reeling under its own surge of coronavirus cases," Times writer Mike Baker wrote. "But in neighboring Idaho, 20 miles down Interstate 90 from Spokane, unchecked virus transmission has already pushed hospitals beyond their breaking point."
Cassie Sauer, the president of the Washington State Hospital Association, told the newspaper while Washington residents are required to wear masks when indoors, students exposed to the virus are required to quarantine, and vaccination orders are in place for many workers, Idaho leaders have issued no such requirements. "It's ridiculous," Sauer said. "If you have your health care system melting down, the idea that you would not immediately issue a mask mandate is just bizarre. They need to be doing everything they can possibly do."
Hospital capacity concerns exist in Idaho and throughout most red states, where Republican governors have sat on their hands for more than a year as much as possible regarding the pandemic.
"Wait times can now be measured in days," CEO Darrell Pile told ProPublica. Pile leads the SouthEast Texas Regional Advisory Council, which oversees patient transfers in a region of 25 counties. State data in the Lone Star State showed only 319 intensive care unit beds available for adults and 104 for pediatric services in the state of some 29 million people. "Now, as the highly contagious delta variant envelops swaths of low-vaccination states all at once, it becomes harder to find nearby hospitals that are not slammed," ProPublica writer Jenny Deam wrote.
Dr. Normaliz Rodriguez, a Florida pediatric emergency physician, told the news nonprofit, "This is not just a COVID issue; this is an everyone issue."
It took doctors six hours to diagnose 12-year-old Seth Osborn with appendicitis after being taken to Cleveland Clinic Martin Health North Hospital in late July, ProPublica reported. Seth's appendix had burst, a life-threatening circumstance, by the time doctors operated on him. Luckily, he survived.
Daniel Wilkinson, a 46-year-old U.S. Army veteran, was not as lucky. Experiencing unbearable pain in his abdomen on August 21, Wilkinson told his mother: "Mama, take me to the hospital." When she did, Dr. Hasan Kakli at Bellville Medical Center in Bellville, Texas, diagnosed Wilkinson with gallstone pancreatitis, an otherwise treatable illness. But doctors couldn't find a hospital with an available intensive care unit bed, ProPublica reported.
Kakli posted on Facebook: "GETTING REJECTED BY ALL HOSPITALS IN TEXAS DUE TO NO ICU BEDS. PLEASE HELP. MESSAGE ME IF YOU HAVE A BED. PATIENT IS IN ER NOW. I AM THE ER DOC. WILL FLY ANYWHERE."
Kakli searched for six hours in Texas, Kansas, Missouri, Oklahoma, and Colorado before a hospital the doctor had contacted earlier found Wilkinson a spot about an hour away in Houston. By that point, the veteran who had served two tours in Afghanistan was in grave condition, his blood pressure dropping, which is a signal of organ failure, Kakli told ProPublica. Wilkinson was flown to the Michael E. DeBakey VA Medical Center in Houston and put in a medically-induced coma, but he ultimately died 26 hours after initially going to the emergency room. "If he had 40 minutes to wait instead of six hours, I strongly believe he would have had a different outcome," told ProPublica.