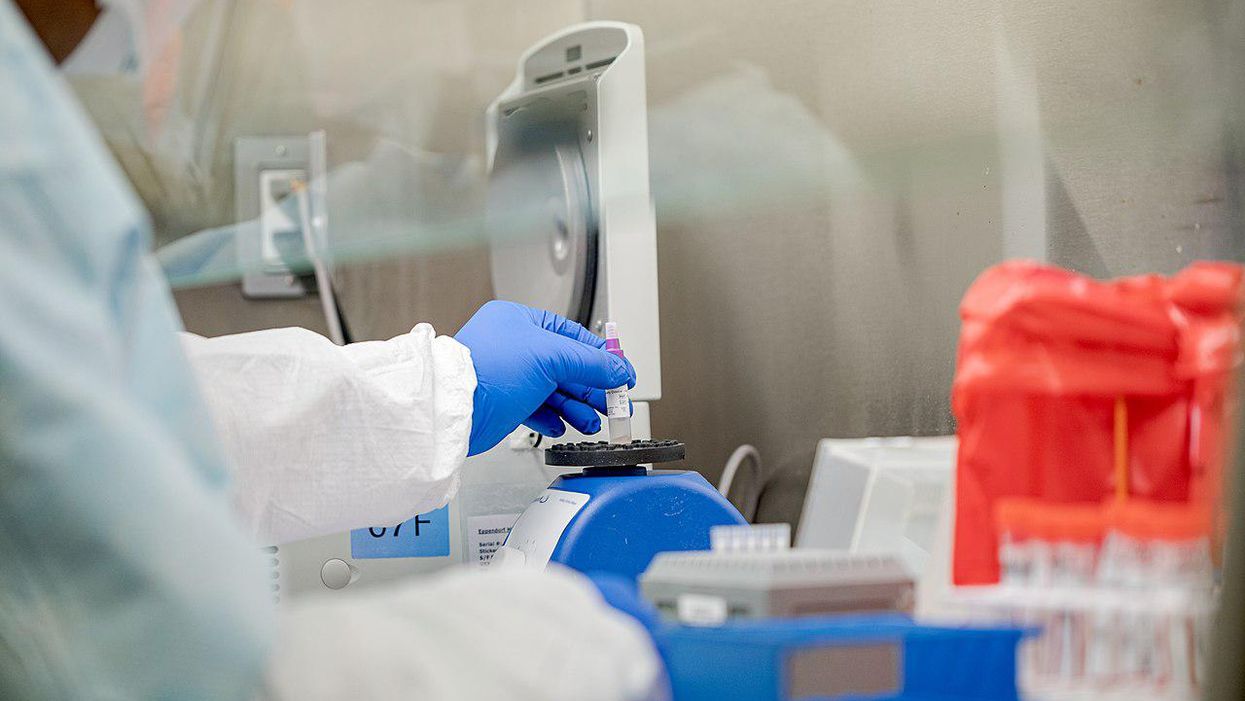
The COVID-19 vaccination rollout in the U.S. is not going well in the majority of states. On Dec. 14 in New York City, Sandra Lindsay became the first American to receive the coronavirus vaccine, ostensibly just one of 20 million scheduled to do so by the end of 2020. Instead, only 3 million Americans had gotten the shot by then, and that number was only up to 4.6 million by Jan. 4. That's barely a one-quarter of the number of doses that had been shipped by then, according to the Centers for Disease Control and Prevention. (Now, in mid-January, almost 1 million doses are being administered per day.)
Dr. Fauci didn't mince words: "(N)o excuses. We should have gotten 20 distributed, and 20 into the arms of people, (and) by 20, I mean 20 million." There's no glib, "WTF" sort of phrase that properly captures how enraging this failure is. The New York Times editorial board called it "an astonishing failure—one that stands out in a year of astonishing failures."
We'll never know how many people in the U.S. will have died or suffered long-lasting harm because we are failing to hit vaccination benchmarks. Yet from the Atlantic to the Pacific, the Great Lakes to the Gulf, we all want to know why we're in this position. Certainly, some of the blame goes to The President Who Tried To Overturn An Election He Lost: Donald Trump refused, for almost a week, to sign the COVID-19 relief bill with over $8 billion earmarked for vaccine distribution—essentially because he was angry about being ignored. Thus, that money couldn't be spent on ramping up the vaccination process for seven extra days—while we all watched the sociopathic Orange Manbaby throw a president-sized tantrum. Prior to Dec. 27, the federal government provided a piddling $340 million for the rollout. As Los Angeles Mayor Eric Garcetti noted, "The federal government can't tell the local governments and state governments to do something and not give us aid."
It's yet another depraved action for which Trump has the blood of Americans on his hands—albeit not on his conscience, as that would require him to have one in the first place. Unsurprisingly, Trump is refusing to accept any responsibility. Again. Instead, he's blaming the states.
Beyond what the soon-to-be-former occupant of the White House did, the vaccine rollout's failures result from thousands of decisions made at the federal, state, and local level by people who, unlike the Insurrectionist-in-Chief, actually have good intentions. Broad reviews of those decisions, and their impact on the delay in vaccinating people, have been written elsewhere. Rather than write another one, I spoke at length with one New York City physician who takes care of patients directly, and who also has significant administrative responsibilities at an ambulatory (outpatient) facility that largely serves Americans of color, most of whom are lower-income.
This doctor, who spoke with me on condition of anonymity, is in charge of securing vaccine doses for their facility, to be administered to health care workers and other eligible staff members. Their facility is not a federally qualified health center (FQHC), which means it has to apply and be formally approved in order to receive the vaccine for its employees; most non-hospitals fall into this category. The physician's experience in seeking approval to receive and administer the vaccine has been, in short, a nightmare. "The whole process has been so stressful and is taking so long," the doctor says. "I want to protect my staff, and I have been working really hard to make that happen, but it is beginning to feel like I am banging my head against the wall."
Non-FQHC facilities seeking the vaccine in New York City must apply to the Citywide Immunization Registry (CIR), while those outside the city go through the New York State Immunization Information System (NYIIS). Non-FQHC facilities throughout the city and state have faced huge hurdles, according to the physician. Their NYC facility, after a month of waiting—while calling or emailing almost daily in pursuit of updates or an explanation for the delay—finally had its application accepted, but then was unable to order the vaccine for another week, due to a problem with the CIR computer system.
The doctor ordered the vaccine about a week into January. As of this writing, they have still not yet been informed when it will arrive. Who knows when they will actually be able to get shots in people's arms? The physician adds: "My staff is getting very antsy; everyone wants to know when we will be getting the vaccine, but I have nothing to tell them. Every day, we email the CIR and get uninformative and evasive responses."
The facility has locations across the state; outside of the city, things are even worse. Six weeks passed before those other locations learned that their applications had been accepted by NYIIS. Like the facility in the city, it remains unclear when those locations might actually receive doses of the vaccine. It's not just New York: Other cities and states are also dealing with delays and problems in getting the vaccine widely administered.
The CIR and NYIIS are significantly understaffed, and admittedly, the holiday season didn't help. Given the COVID-19 crisis, it is an open question as to whether staff should have been asked to continue working over those holidays and/or over weekends—with proper compensation, of course. New York City and state alike would've needed financial help to pay those workers—help that did not arrive in time, thanks to the whims of a certain Individual-1.
Independent doctors' offices and freestanding medical facilities face additional barriers to acquiring the vaccine for their employees. "The process has been extremely difficult, opaque and time-consuming," the clinic doctor relates. "I cannot imagine how an organization smaller than ours would ever be able to do it."
They can't, they won't, and they don't. As the physician I spoke to explained, many of these smaller facilities simply won't bother to apply for various reasons, including, but not limited to:
- Many facilities are already short-staffed because of COVID-19, so they don't have the staff to deal with the application process and/or to administer the vaccine, as well as comply with the incredibly stringent post-vaccination reporting requirements;
- Facilities don't have appropriate storage, particularly cold storage, for the vaccine;
- The minimum number of doses a single facility can receive—the 100 doses in a Moderna box—far exceeds the number of employees at most of these facilities, leading to concerns about wasting doses that are needed elsewhere.
On that last point, there's another concern. Initially, there was some confusion about whether Gov. Andrew Cuomo's threat—to slap a $100,000 fine on any hospital that doesn't use all doses issued within seven days—also applies to smaller health care facilities and practices. Numerous physicians and health care administrators told The New York Times that this lack of clarity and fear of financial penalties discouraged smaller facilities from applying if they didn't have enough eligible staff to receive vaccinations. Given that the minimum number of doses a facility can order is 100, what happens if a facility only has 50 eligible employees, or 20?
Cuomo seems to have since "softened" the threat of a large fine, and clarified that facilities can send excess vaccine doses back to the state; given storage requirements—the Pfizer vaccine must be stored at -70° C—that still may present difficulties for many facilities.
If employees at smaller facilities can't get vaccinated at work, they will further burden any alternative delivery system—systems that currently are unable to handle the load they already have. Many local health departments have set up vaccination sites for health care workers, but these sites are few and far between, and appointments are difficult to get. And, how will already understaffed facilities cope with employees missing time to chase down their shots? The questions go on and on.
The New York City doctor's experience tracks with the broader failure of the city and state's vaccination rollout. Seventeen days in, barely 88,000 NYC residents had been vaccinated—1% of the population in a city as hard hit as any place in the world, where the current positive test rate stands at almost 1 out of 10. Scarily, vaccinating large numbers of people is only going to get harder, as The New York Times reports.
The pace is worrying some experts. "I do feel concern," said Dr. Wafaa El-Sadr, an epidemiology professor at Columbia University. Despite months to prepare, there still seemed to be a steep learning curve when it comes to "the nitty-gritty of how do you get it from the freezer to the arm as quickly as possible," she said. "I think there are growing pains as people are picking up how to do this."
The first phase should have been the simplest, she added. "We've started out with the easiest populations, an almost captive audience: nursing homes and hospital workers — you know who they are and where to find them."
The problems faced by non-hospitals, as reported by the NYC doctor, are echoed in the Times' analysis.
"We feel forgotten," said Dr. Kerry Fierstein, a pediatrician and chief executive of a company that runs pediatrician offices, mainly on Long Island and in New York City. "If you're owned by a hospital, you've probably been vaccinated, but if you're completely unaffiliated, you don't know when you'll get vaccinated."
More broadly, the barriers non-hospital employees face in getting access to the vaccine mirror and exacerbate larger health care and societal inequalities in the U.S. relating to race, education, and class—inequalities that are particularly acute for COVID-19. In many cases, physicians in medical practices are able to be vaccinated at the hospital where they admit patients, but only as individuals. Think of the medical assistants, phlebotomists, and front desk workers at these facilities—all of whom interact with patients directly—as well as the cleaning staff and others who are also at risk. None of them can get the vaccine at work until their facility goes through the onerous process described above, actually gets approved, and decides to follow through and order the vaccine (then receives it). These workers, along with home health aides and others working for agencies, are also more likely to be women, and more likely to be Black or brown.
Lower Black and brown vaccination rates are a particular concern due to the disproportionate impact COVID-19 has had on those communities. The lower rates result in part from long-standing (and well-founded) mistrust of the medical establishment and the government when it comes to vaccines and other health issues.
The doctor I spoke to suggested that, in order to get more Black and brown health care workers to take the vaccine, we need to offer it to them in their own workplaces, delivered by medical providers and staff with whom they feel comfortable discussing their vaccine hesitancy—people they know and trust: "I have had conversations with individual staff members who were hesitant about getting the vaccine. I was able to take the time and answer their questions—after which almost all of them decided to be vaccinated with us, because they know and trust me and our organization. They would not feel comfortable being vaccinated at a large, unfamiliar, and impersonal venue." Just one more reason to offer the vaccine in workplaces whenever possible.
Hopefully, New York and the other cities and states will share information and learn from one another about what went wrong—even as they're working feverishly to vaccinate people. "It's gone too slowly, I know, for many of us," acknowledged California Gov. Gavin Newsom shortly after New Year's. "All of us, I think, want to see 100% of what's received immediately administered in people's arms. That's a challenge."
On Jan. 5, Cuomo introduced a revised vaccination plan for New York, conceding that the existing approach wasn't working. The new plan has three components: First, vaccinate all staff and residents in nursing homes, over a two-week period. Next, a push to get hospitals to vaccinate their health care workers; and finally, "special efforts" created by the state to directly deliver shots to all eligible New Yorkers. These efforts include drive-through vaccination locations and pop-up locations in houses of worship and community centers. There's also a special focus on social equity, and making sure that Black and Latino New Yorkers get their shots.
The situation remains fluid as of this writing. Multiple rounds of changes have been issued in recent days. Taken together, they have broadened the eligibility criteria for receiving the vaccine to include all New Yorkers over the age of 65, those who are immunocompromised, and some essential workers—including K-12 teachers!
The clinic doctor remains frustrated by the continued delays in getting their facility's staff vaccinated, and it's not clear how much the revised distribution approach will help non-hospital health care workers access the vaccine more quickly ... if at all. As for whether Cuomo's new plans address these concerns and improve the overall vaccination situation in New York? Only time will tell.
Ian Reifowitz is the author of The Tribalization of Politics: How Rush Limbaugh's Race-Baiting Rhetoric on the Obama Presidency Paved the Way for Trump (Foreword by Markos Moulitsas)